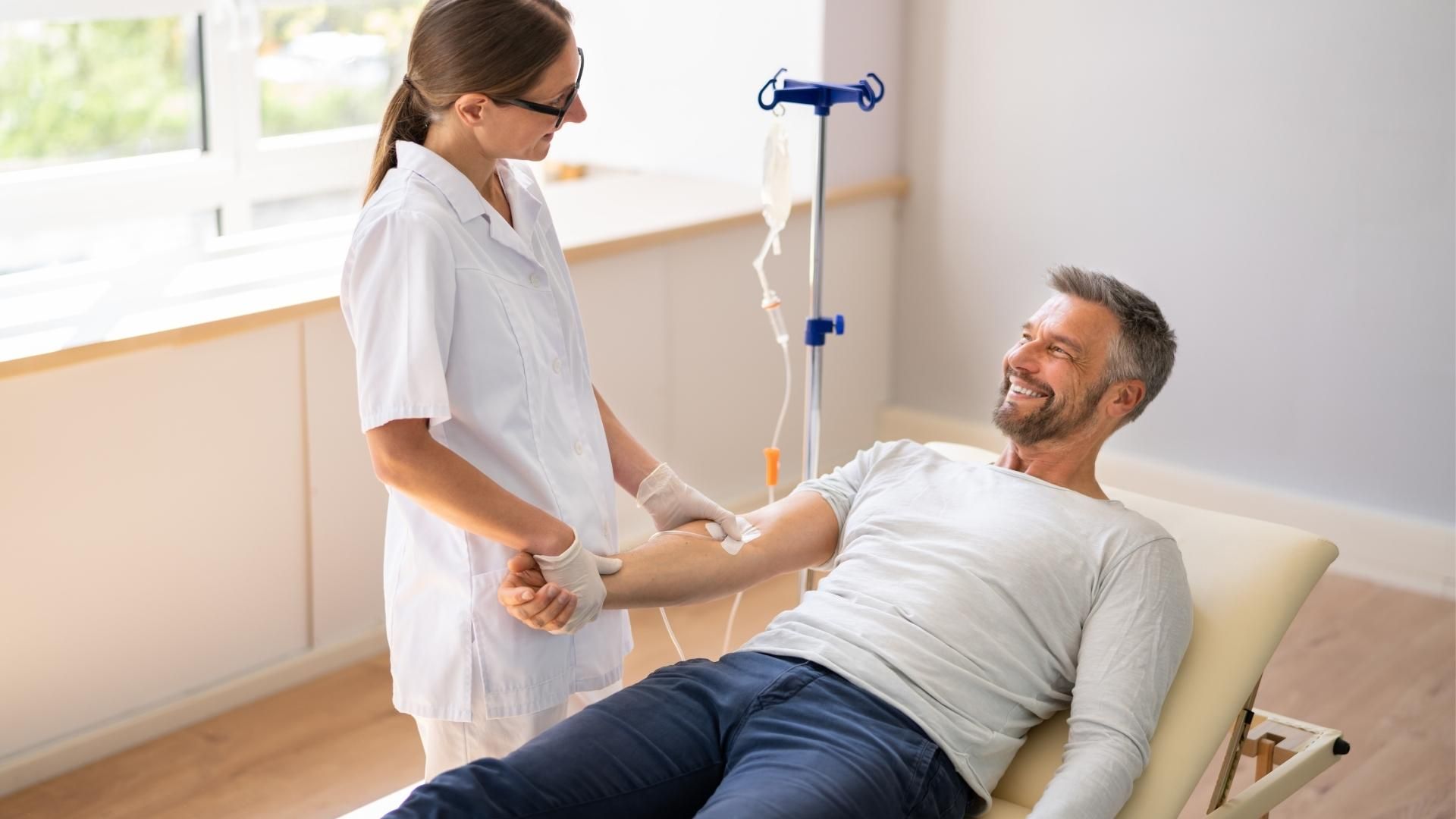
Comfort During Long Home Infusions: How to Plan Your Setup and Feel Better
Some home infusions take 30 minutes. Others take four, six, or eight hours. For patients on longer therapies, IV days can feel physically and emotionally demanding. That doesn't mean something is wrong, but it does mean comfort is worth planning for deliberately.
This guide helps you think through the physical setup, the symptom tracking, and the practical small details that can make a long infusion day easier to manage.
Key Takeaways
- Positioning matters more during long infusions than most patients expect.
- Small setup decisions made before you start can reduce unnecessary movement and stress throughout the session.
- Symptom tracking becomes more useful during long infusions because timing matters clinically.
- If anything feels new, worsening, or unclear, call your Pharmko care team before deciding it's nothing.
How to Set Up for Comfort Before You Start
Choose Stable, Sustainable Positioning
Before you begin, think about where you'll sit or rest and whether you can realistically stay there for the full duration. A setup that feels fine for 20 minutes may become frustrating or painful after several hours.
Ask yourself:
- Can I stay in this position comfortably for the full session?
- Can I reach essentials without pulling on tubing or shifting too much?
- Can I see or check my line site without major repositioning?
If the answer to any of those is "probably not," adjust before you start, not mid-infusion.
Place Essentials Within Reach
Long infusions feel more manageable when the things you need are already nearby before the first drop runs. Consider having the following within easy reach:
- Water or approved hydration, if allowed
- Your phone and charger
- A light blanket or extra layer
- A notebook or notes app for symptoms and questions
- Your Pharmko contact number
Start With a Clean Workspace First
Comfort shouldn't come at the expense of organization.
Your clean workspace routine should happen first, then build your comfort setup around it.
What to Track During a Long Infusion
Timing and Symptom Onset
The most useful information you can give your care team isn't just what you felt, but when it changed. A symptom in the first 10 minutes may mean something different than one that appears four hours into a session. That timing context helps your care team assess what's happening and respond accurately.
A simple log works well:
- Infusion start time
- What changed
- When it started
- Whether it stayed the same, improved, or got worse
What Normal Fatigue Looks Like Versus What Requires a Call
Feeling tired during a long infusion can be normal. The following symptoms are not, and should prompt a call to your Pharmko care team rather than a wait-and-see approach:
- Chills or fever
- Shortness of breath or chest discomfort
- Redness, swelling, warmth, or drainage at the line site
- Dizziness, lightheadedness, or near-fainting
- A headache that feels new or significantly worse than usual
Your red-flag symptom guide should be easy to access before every long infusion session, not something you search for after a symptom appears.
How to Make a Long Infusion Day More Manageable
Plan Low-Effort, Low-Movement Activities
Audiobooks, podcasts, music, and shows that don't require physical movement are ideal for longer sessions. They help the time pass without encouraging too much shifting, repositioning, or arm movement that could disturb your line or tubing.
Keep Your Questions Organized
Long infusions are often when patients notice patterns or questions they'd otherwise forget by the time their next check-in arrives.
An organized home infusion guide gives you a dedicated place for those notes so follow-up conversations with your care team are more focused and useful.
What You Can Do Today
- Test your infusion position in advance and assess whether it's actually sustainable for your full session length.
- Create a simple symptom note format with time, change, and severity so tracking during your next long infusion is automatic.
- Set up a small comfort station with the items you usually need nearby before your next session.
- Review your pump and supply basics so equipment behavior during a long session doesn't feel unfamiliar.
Safety Note
This content is for education only and does not replace clinical guidance from your Pharmko care team. Fatigue and mild discomfort may happen during longer infusions, but anything new, escalating, or concerning should be discussed before you decide it's nothing. If symptoms feel severe or immediately dangerous, contact emergency services.
FAQs
What if I feel uncomfortable but I'm not sure whether it warrants a call?
Call your Pharmko care team. The definition of "uncertain" in a medical context is always a reason to reach out rather than wait.
Can I move around during a long infusion?
This depends on your therapy, pump type, and line. Your Pharmko nurse will give you specific guidance during training. Generally, limited and careful movement is often possible, but it should be planned with your setup in advance, not decided spontaneously mid-session.
How do I track symptoms without overanalyzing every sensation?
Focus on what's new or different from your baseline. You don't need to document every moment, just what changes, when it changes, and whether it's getting better or worse.
Related Reading
- Home infusion clean workspace setup
- Infusion pumps and supplies 101
- When to call your care team: red flags during infusion