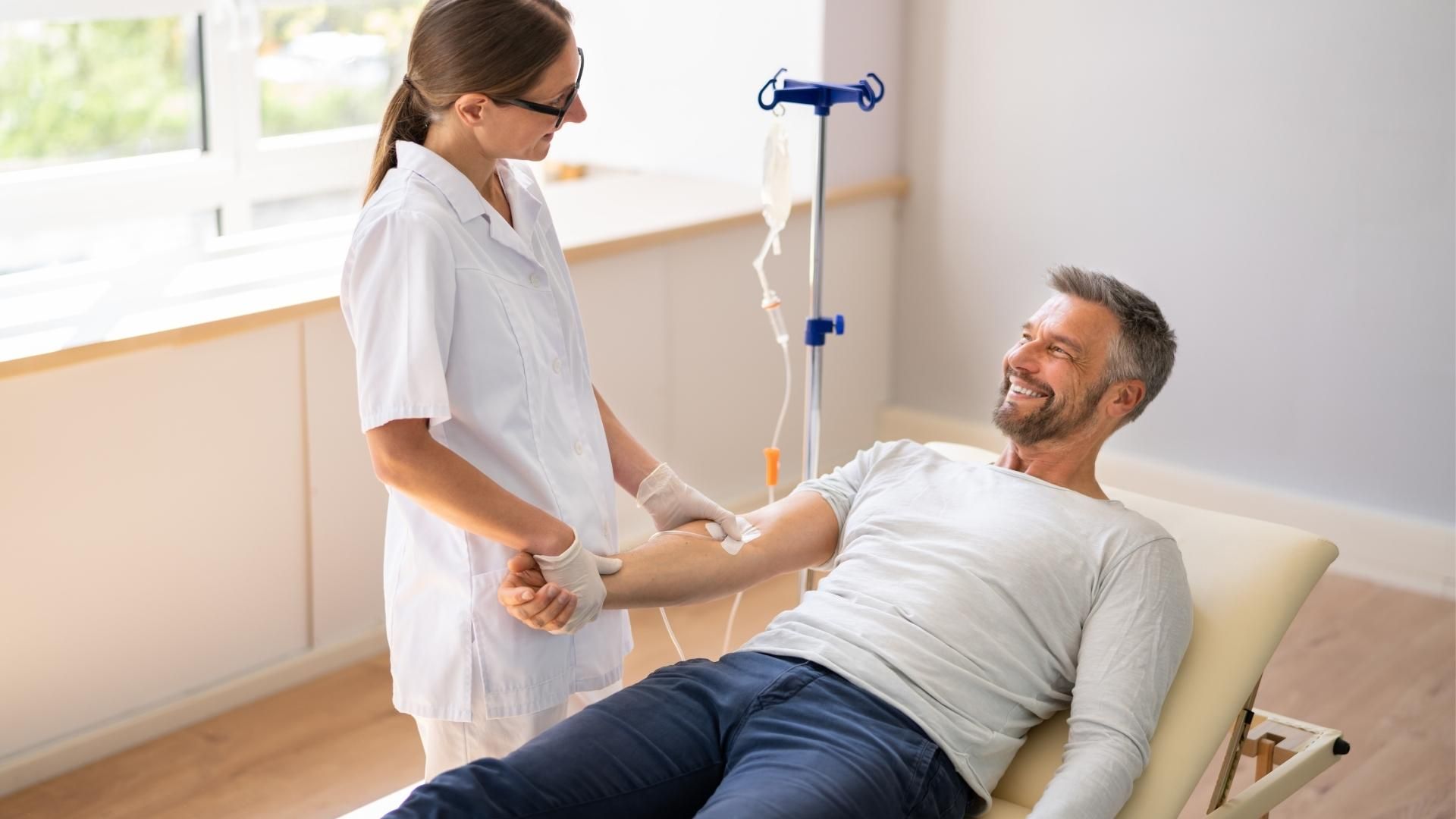
Work and School While on Home Infusion: Scheduling, Planning, and What to Ask For
Many patients continue working, attending school, or maintaining active daily routines while on home infusion therapy. It's not only possible, for many people, maintaining normalcy is part of what makes home infusion preferable to other care settings in the first place. But doing it safely requires a few deliberate decisions: choosing the right infusion window, planning supplies reliably, and knowing what to do when something changes outside your usual support hours.
This guide helps you think through each of those areas practically.
Key Takeaways
- A consistent infusion window that fits your schedule is something your care team can help you build, but only if you ask. Bring your actual schedule to that conversation.
- Supplies and deliveries need more lead time than most active patients plan for. Don't reorder reactively.
- After-hours planning is especially important when questions or symptoms arise during workdays, school evenings, or weekend commitments.
- If symptoms appear while you're working or in class, they follow the same red-flag rules. Location doesn't change clinical urgency.
Building a Routine That Fits Real Life
Choose an Infusion Window You Can Consistently Protect
The most important scheduling decision you'll make is choosing when your infusion happens. The goal is a window that:
- Falls at a consistent time each day or week, because consistency protects against missed steps
- Is predictably available, not dependent on variable conditions
- Allows for the full infusion duration without rushing
- Gives you a buffer before and after for setup and cleanup
Common approaches patients use:
- Before work or school: Morning infusions work well for patients who can protect the hour before they leave.
- Evening or overnight: Many patients schedule longer infusions to run while they sleep, especially TPN and certain nutritional therapies.
- Midday break: Some patients manage daytime infusions during a lunch window or free period if duration allows.
Bring your actual schedule to your Pharmko care team when discussing options. Some therapy types have more scheduling flexibility than others, and your care team can tell you what's safely adjustable for your specific medication and route.
Use a Checklist to Reduce Decision Fatigue
When you're managing a morning infusion before a workday, you don't have mental bandwidth to reconstruct your setup steps from memory.
A first-dose checklist approach establishes your setup as a fixed sequence you follow rather than rebuild each time, which reduces both errors and stress.
Print your checklist and post it in your infusion area. Use it every time, even when you feel like you don't need to.
Planning Supplies and Deliveries Around Your Schedule
The Logistics Problem That Trips Most Active Patients
Patients who maintain active schedules often encounter the same problem: they realize they're low on supplies on a day when they have no time to manage a call, a shipment is delayed, or an insurance authorization has lapsed. These issues compound quickly.
The solution requires a discipline shift: treat supply planning like a standing appointment rather than a reactive task. Your refill and delivery planning guide walks through the weekly inventory check system that prevents this pattern before it starts.
Build Delivery Lead Time Into Your Calendar
Insurance-required prior authorizations, processing times, and shipping logistics all add days to a refill cycle. If you're reordering when you feel low, you're already at risk.
The practical rule: when you have approximately two weeks of doses remaining in supplies, initiate your reorder. That window absorbs delays without creating a therapy gap.
What to Do If Symptoms Change During a Workday or School Day
Red-Flag Rules Don't Change Based on Location
A symptom that would require a call at home also requires a call at work. Fever and chills, rash or hives, shortness of breath, or significant line site changes don't become less urgent because you're in a meeting or a classroom.
Know your red-flag symptoms in advance so you can recognize and respond immediately, regardless of where you are. If your infusion window is in the morning before work, your most likely symptom window is during your workday, not at home.
Have Your After-Hours Pathway Ready for Evenings and Weekends
If your infusion falls in the evening or if you're managing therapy during a weekend schedule, you need an after-hours plan in place before you need it. After-hours home infusion support covers exactly what to have ready: your contact pathway, your therapy details, and what constitutes a call-now versus a call-in-the-morning situation.
What You Can Do Today
- Block your infusion window on your calendar and treat it as non-negotiable.
- Create a one-page reference sheet with your therapy name, dose schedule, and Pharmko contact number that you can keep at your desk or in your bag.
- Set a weekly supply check reminder for a fixed day, put it in your calendar like any other appointment.
- Talk to your Pharmko coordinator about scheduling flexibility if your current window isn't working. There may be options you haven't explored yet.
- If you're returning to work or school after a hospital discharge, make sure your hospital-to-home transition addressed scheduling and logistics explicitly, not just the clinical handoff.
Safety Note
This content is for education only and does not replace clinical guidance from your Pharmko care team. Any changes to your infusion schedule, including timing and frequency, must be approved by your prescribing physician and coordinated with your Pharmko nurse before implementation.
FAQs
Can I adjust my infusion timing to fit my work schedule?
Sometimes, yes, but only with your care team's approval. Some medications have specific timing requirements; others offer more flexibility. Bring your actual schedule to the conversation. Your Pharmko coordinator can tell you what's possible for your specific therapy.
What if I feel symptoms while I'm at work or in class and I'm not sure it's serious?
Use your red-flag reference and call your care team. If symptoms feel severe, such as difficulty breathing, chest tightness, or fainting, call emergency services first, then call Pharmko. Location doesn't reduce urgency.
What if I'm feeling overwhelmed managing work and a new therapy at the same time?
That's a common experience in the weeks following a transition from inpatient to home therapy. The hospital-to-home transition guide addresses how to set realistic expectations for that adjustment period and what kinds of support you can ask for.
Related Reading
- Hospital-to-home transition for home infusion
- Starting home infusion: first-dose checklist
- After-hours home infusion support