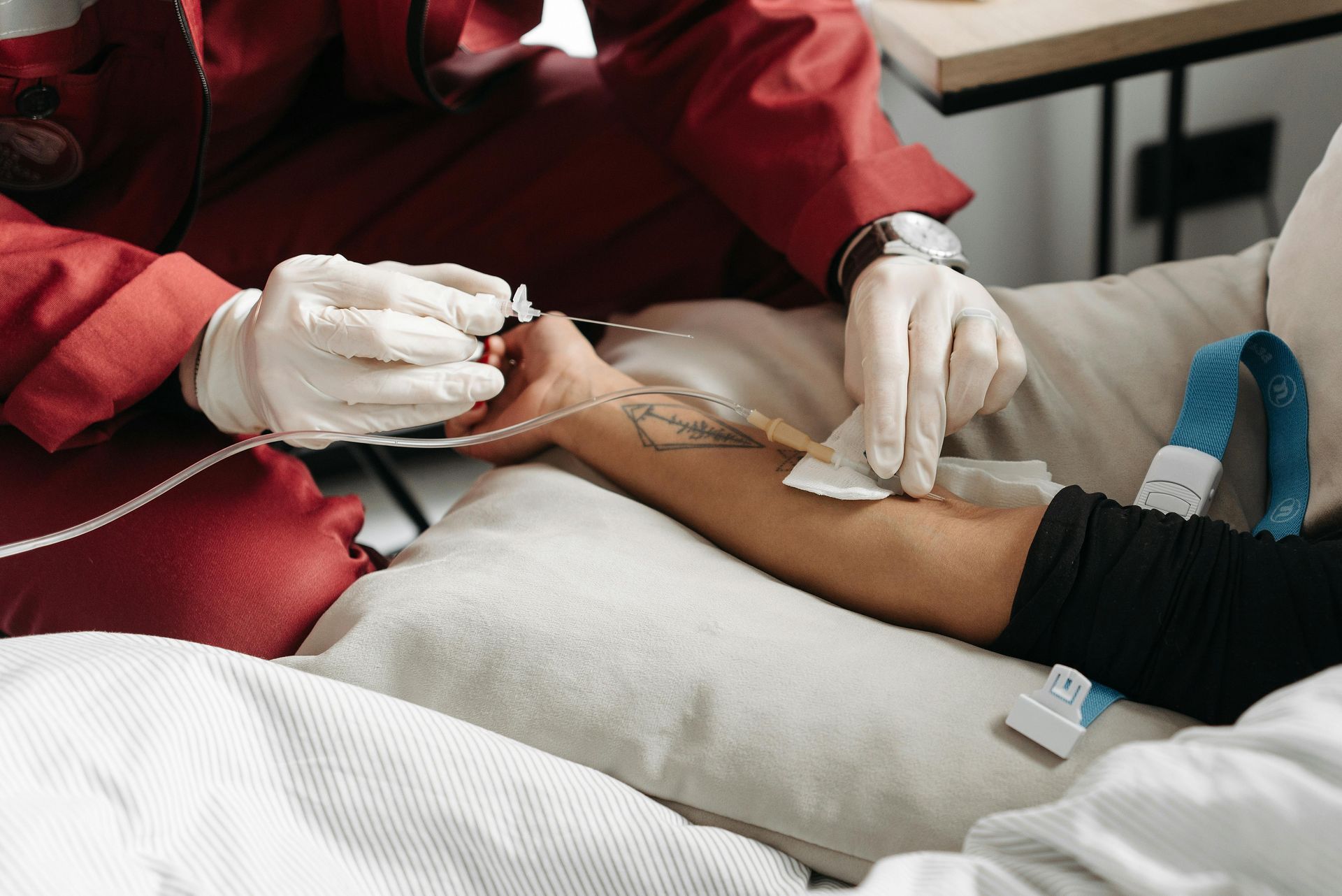
Malnutrition in Hemodialysis Patients: Signs, Risks, and When IDPN Is Needed
Malnutrition is one of the most prevalent and consequential complications in patients receiving hemodialysis. Research estimates that protein-energy wasting (PEW) affects between 28% and 75% of dialysis patients depending on the population and criteria used. Despite this prevalence, it remains underdiagnosed and undertreated in many dialysis settings. Pharmko supports dialysis clinics with IDPN and renal nutrition services designed to close this gap.
Why Hemodialysis Patients Are at High Nutritional Risk
Hemodialysis patients face a combination of factors that collectively drive nutritional decline:
- Inadequate dietary intake due to uremia-related anorexia, dietary restrictions, and nausea
- Nutrient losses during each dialysis session , amino acids and water-soluble vitamins
- Chronic systemic inflammation driven by uremic toxins and the dialysis process itself
- Metabolic acidosis, which accelerates protein catabolism
- Comorbidities including diabetes, cardiovascular disease, and infections
Recognizing Protein-Energy Wasting: Clinical Indicators
The ISRNM defines PEW by the presence of abnormalities in at least three of four categories:
1. Biochemical markers
- Serum albumin < 3.8 g/dL
- Serum pre-albumin (transthyretin) < 30 mg/dL
- Serum cholesterol < 100 mg/dL
2. Body mass
- BMI < 22 kg/m²
- Unintentional weight loss of 5% over 3 months or 10% over 6 months
3. Muscle mass
- Reduced mid-arm muscle circumference
- Muscle wasting visible on physical exam or confirmed by imaging
4. Dietary intake
- Low protein intake (< 0.8 g/kg/day) for at least 2 months
- Low energy intake (< 25 kcal/kg/day)
The Clinical Consequences of Untreated Malnutrition
PEW in dialysis patients is independently associated with increased risk of hospitalization, higher infection rates, cardiovascular complications, reduced functional capacity, and higher all-cause mortality. Correcting malnutrition has been shown to improve survival outcomes, reduce hospitalizations, and improve patient-reported quality of life.
The Stepwise Approach to Nutritional Support
Clinical guidelines recommend a stepwise approach before escalating to parenteral nutrition:
- Step 1: Dietary counseling and individualized meal planning
- Step 2: Oral nutritional supplementation (ONS) , high-protein, renal-appropriate supplements
- Step 3: Intradialytic parenteral nutrition (IDPN) when ONS fails after 2–3 months and albumin remains below 3.5 g/dL
- Step 4: TPN for patients who cannot absorb adequate nutrition enterally
For a detailed breakdown of IDPN eligibility criteria, administration, and the referral process, see our dedicated guide on who qualifies for IDPN and how it works.
How Pharmko Supports Renal Nutrition
Pharmko's renal nutrition team , including clinical pharmacists and registered dietitians , works directly with the dialysis care team to evaluate eligibility, prepare custom IDPN formulations, coordinate insurance authorization, and monitor clinical response. We deliver IDPN solutions directly to dialysis centers and adjust formulas based on lab trends and clinical changes.
→
Refer a patient or contact our renal nutrition team:
1-877-549-3863